by Mike Thurber, Principal Scientist, Elder Research

Three weeks ago, our Brief Is the Spread of the COVID-19 Coronavirus Being Slowed looked at the impact of social distancing on the flu. Evidence showed that the unprecedented measures taken by the government are having the expected effect, as measured by seasonal flu cases. In this Brief, we update and amplify that information.
The economic costs of social distancing are enormous, so we need to quantify the health benefits, even if only roughly. Each new set of data lets us delve deeper into the impact on the flu season. Here, we will look at positive flu test results, drill into its different strains, and review hospitalizations. Because deaths lag new case reports by about four weeks, it is still too early to see the effect of social distancing on flu death rates.
Flu Cases
Figure 1 shows weekly positive flu test trajectories for the last 10 seasons. Recent data confirms the prior conclusion that social distancing and other mitigation measures have blunted the 2020 flu season (thick black line):
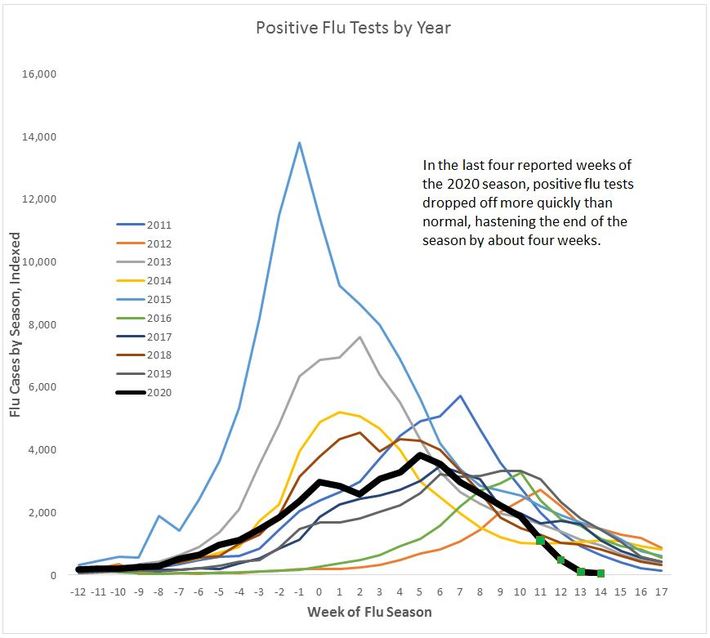 Figure 1: Reported Flu cases by season by week. Cases in 2020 dropped after week 10, ending the flu season earlier than prior seasons. (Data adjusted from CDC.gov Flu Weekly web site)
Figure 1: Reported Flu cases by season by week. Cases in 2020 dropped after week 10, ending the flu season earlier than prior seasons. (Data adjusted from CDC.gov Flu Weekly web site)
To estimate the impact, let’s compare the current season to the 2013 flu season, when the level of new cases was approximately the same at week 10. In 2013, weeks 11+ saw about 48,000 new cases in the U.S. In 2020, if rates remain at their current level, there will be only 15,000 new flu cases for the same period – a 68% reduction. If we follow this with the observed ratio of deaths to reported cases, we estimate roughly 1,000 deaths from flu will be saved in the 2020 season due to COVID-19 social distancing.
Will the response of COVID-19 to social distancing be similar? COVID-19 is a novel respiratory virus, so, of course we don’t have prior data for it. We do, however, have data on the many different strains of the flu, and can see if they are all equally affected by social distancing. Different strains have different levels of prevalence each year, so we need to normalize them as the percent of each strain’s average for the year. We take 2019 as an example, where there is considerable variety among the strains’ trajectories, with H1N1 dying off more quickly than the others.
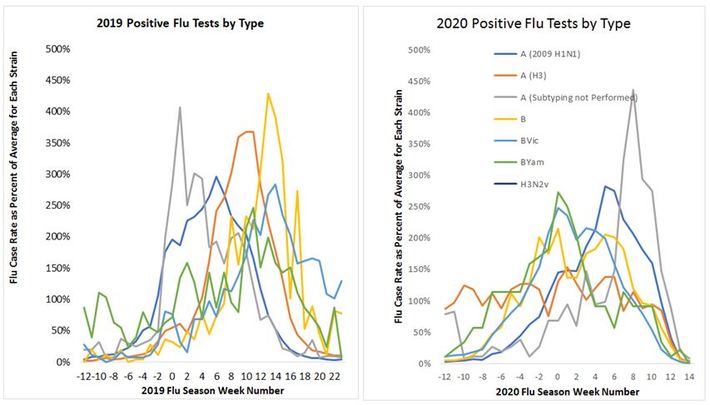 Figure 2a&b: 2019 & 2020 Flu Case Rates by Strain. In 2019 flu strain trends are divergent throughout season; in 2020 they are divergent then drop together with social distancing (we are now at week 14).
Figure 2a&b: 2019 & 2020 Flu Case Rates by Strain. In 2019 flu strain trends are divergent throughout season; in 2020 they are divergent then drop together with social distancing (we are now at week 14).
2020 flu strain trends are similarly divergent until social distancing (starting week 10), at which point they drop off in tandem to almost nothing. This strongly suggests that the social distancing measures implemented in the US have proven effective for multiple strains of flu, adding to our confidence that they will work for COVID-19.
Hospitalizations
Flu hospitalizations show the same retarding effect of social distancing as do cases. Figure 3 shows the hospitalizations by season, normalized to peak at 100%, with the peak week defined as week zero. Note that the current year dropped precipitously 5 weeks after its peak, and is lower at 8 weeks after the peak than any of the prior ten years.
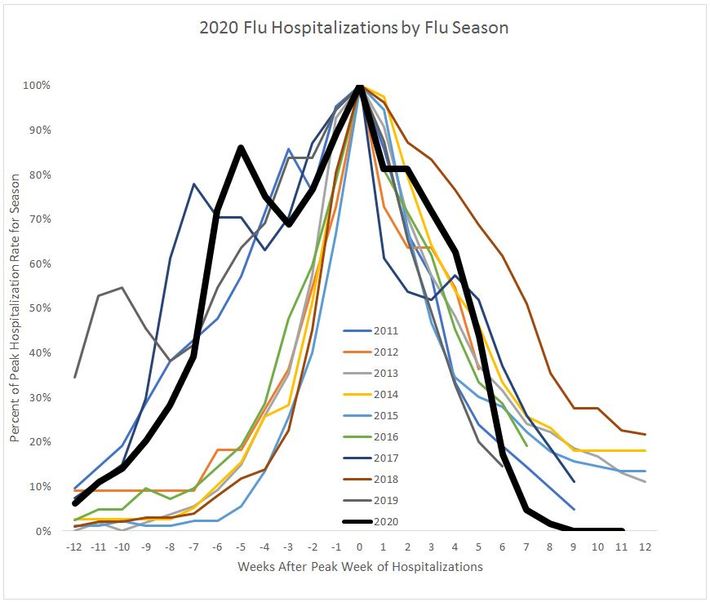 Figure 3: Relative Hospitalizations due to flu by year (Data adjusted from CDC.gov Flu Weekly web site)
Figure 3: Relative Hospitalizations due to flu by year (Data adjusted from CDC.gov Flu Weekly web site)
If hospitalizations are reduced to the same extent as cases — 68% — we can expect roughly 7,500 fewer flu hospitalizations for the 2020 flu season due to COVID-19 social distancing.
Conclusion
A fortunate byproduct of COVID-19 social distancing policies has been a sharp reduction in flu cases and hospitalizations, both of which dropped more precipitously than in any recent season, soon after social distancing guidelines were instituted. This has been shown to be true for all reported strains of the flu. This finding encourages us that these policies are likely also effective in mitigating the spread of COVID-19, where measuring the effect is much more difficult, due to the novelty of the virus. We urge leaders to use the hard-won time wisely, using analytics to inform public policy to save lives and livelihoods alike. A discussion of how to more directly measure the effect of social distancing on mitigating the spread of COVID-19 will be a subject of a coming brief.
