
- A hundred years of modeling didn’t help forecast the extent of the current pandemic.
- Hundreds of thousands of deaths could have been prevented with better models.
- The quantitative economic epidemiological model may be the future for pandemic modeling.
Many countries, including the UK and US, mounted inefficacious responses to the Covid-19 pandemic, thanks to inaccurate and delusive models. No one saw how badly the pandemic would affect social and economic constructs; WHO director General Tedros Ghebreyesus remarked early in the pandemic that …none of us could have imagined how our world and our lives would be thrown into turmoil by this new virus [1].
Standard epidemiological models for Covid-19 were off by wide margins and some predictions were wrong by at least an order of magnitude [2]. The disease spread faster than the models predicted, resulting in hundreds of thousands unnecessary deaths and delayed lockdowns [3]. Meanwhile, other countries like China, who didnt rely on epidemiological models based on 100-year-old data, demonstrated effective pandemic control with case management, contact tracing, and lockdowns [4].
The fact that models failed so spectacularly doesnt mean that modeling is doomed. However, the standard epidemiological models may have seen their day. Future models are likely to incorporate a variety of socioeconomic factors, with input from economists as well as epidemiologists.
The Failure of Standard Models
The failure of standard epidemiological models was the result of multiple factors, including over-reliance on disease models as a substitute for the human element of pandemic engagement. Epidemiology-based models cant capture the trade of between health (e.g., adhering to self-isolation guidelines) and economic well-being (e.g., the need to work).
Policies based on the standard epidemiological models dont always reflect everyday reality or predict how individual preferences affect behavior and the spread of disease [5]. For example, one widely known modelR-naughtis an indicator of how many people one infected person can be expected to transmit a disease to. While R-naught is a useful tool for modeling the spread of the virus and effectiveness of vaccines, it does not tell us whether lockdowns are economically feasible from a private or public standpoint. It doesnt tell us what we can do to prevent another pandemic from happening again, how people will behave during a new pandemic, or when the current pandemic purgatory will end.
Is the solution a quantitative economic epidemiological model?
One solution offered by several economists is to devise a pandemic model that is based on an interaction between the spread of disease and societal behavior. These models aren’t new: quantitative epidemiological models had already been developed well before the current pandemic.
One of the pioneers of the social model of disease model was Tomas Philipson, who studied how behavior and the spread of disease interacted during the HIV/AIDS pandemic [6]. Philipson argued that individual behavior to prevent transmission of disease is self-limiting: at first, people will alter their behavior to avoid catching the disease; But when the numbers of infected fall, people slip back into pre-disease habits and the disease reemerges. The standard traditional models would not have taken this, or any other aspect of private behavior, into account. However, quantitative epidemiological models, that include a behavioral response to disease prevalence, may be more useful for evaluating the impact of public health interventions and societal reactions to the emergence of new virus strains. One such model, developed by UCLA researcher Andrew Atkeson, closely follows the behavioral model of daily deaths in the US [7]:
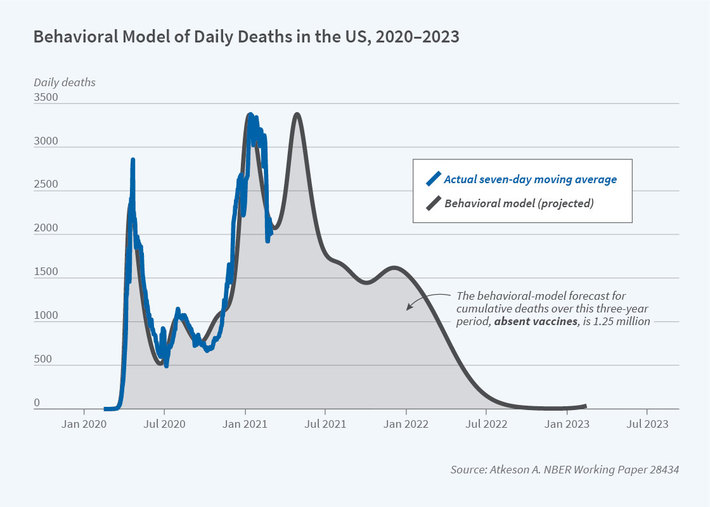
To be useful in advising policy makers, states Atkeson, models need to capture how individual choices interact with economic output and the spread of disease. There is a pressing need for improved models; While many scientists expect COVID-19 to become endemic [8], studies tell us another pandemic will hit in our lifetime [9]. Lets hope were ready.
References
Image: Covid-19 Graph: Adobe Creative Cloud (Licensed).
[1] WHO Director-General’s opening remarks at the media briefing on COV…
[2] COVIDs Lessons for Future Modeling of Pandemics
[3] Imagining pandemics now, and then: a century of medical failure
[4] Here are five ways the government could have avoided 100,000 deaths.
[5] Private Choices and Public Health
[6] Modeling Behavior during a Pandemic: Using HIV as an Historical Ana…
[7]. A Parsimonious Behavioral SEIR Model of the 2020 COVID Epidemic in …
[8] The coronavirus is here to stay heres what that means
[9] Statistics Say Large Pandemics Are More Likely Than We Thought
